What Is Multiple Sclerosis?
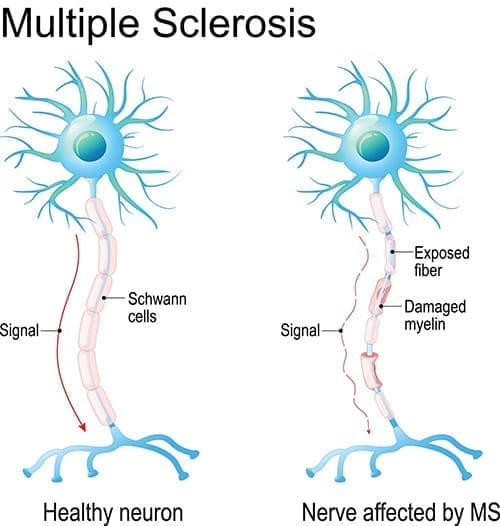
Multiple sclerosis (MS) is an autoimmune disease that affects the nervous system, launching an attack on its own tissue. Multiple sclerosis can range from relatively benign to somewhat disabling to devastating, as communication between the brain and other body parts is disrupted. Multiple sclerosis affects balance, coordination, strength, and other body functions to varying degrees based on severity and form.
What are the symptoms of Multiple Sclerosis?
Understanding the multifaceted nature of multiple sclerosis (MS) symptoms is crucial for those navigating this complex condition. MS manifests in various ways, and its symptoms can fluctuate in intensity and duration. Here’s a more detailed exploration of the common symptoms associated with MS:
- Weakness and fatigue: Individuals with MS may experience weakness, especially in the limbs. This fatigue can be both physical and mental, impacting daily activities.
- Tingling and numbness: Sensations of tingling or numbness, often described as pins and needles, can occur in different parts of the body, reflecting the disruption in nerve signals.
- Poor balance and coordination: MS can affect the cerebellum, leading to difficulty maintaining balance and coordination. This can result in unsteady movements and an increased risk of falls.
- Visual disturbances: Blurred or double vision and pain or discomfort during eye movement may be indicative of MS affecting the optic nerves.
- Vertigo and dizziness: Some individuals may experience dizziness or vertigo, which can further impact balance and spatial orientation.
- Muscle spasms and tremors: Involuntary muscle spasms and tremors are common in MS. These can range from mild to severe, affecting mobility and comfort.
- Cognitive changes: MS can influence cognitive functions, leading to difficulties with memory, concentration, and overall mental sharpness.
- Bladder and bowel issues: Dysfunction in the nerves that control the bladder and bowel can result in issues such as incontinence, urgency, or difficulty with bowel movements.
- Emotional changes: Mood swings, depression, and anxiety are not uncommon in individuals with MS, possibly linked to the challenges posed by the condition.
- Pain: Chronic pain, often affecting the back or limbs, is a symptom that some individuals with MS may experience.
How is Multiple Sclerosis diagnosed?
Navigating the path to an accurate MS diagnosis involves carefully examining symptoms and considering the diverse nature of this condition.
- Blood tests: A series of blood tests will be carried out to help rule out other conditions that may present with symptoms similar to MS, such as Lyme disease.
- Measuring nerve signal speed: A pivotal step in the diagnostic process is measuring nerve signal speed. This test provides valuable insights into the functioning of your nervous system.
- MRI scan: To better understand the impact on the nervous system, patients may be given an MRI. This advanced imaging technique allows doctors to meticulously examine brain images, identifying areas of potential damage.
Spinal tap: A spinal tap, or lumbar puncture, is a diagnostic tool that offers a closer look at the fluid flowing in the brain and spinal cord. This examination helps unveil signs that the immune system may inadvertently harm the nervous system, a characteristic feature of MS.

What causes multiple sclerosis?
The causes of multiple sclerosis remain unknown. MS showcases geographical variations, with higher prevalence in regions like Scotland, Scandinavia, and northern Europe. In the U.S., a distinct pattern emerges, where the occurrence is more common among white people of European descent. Multiple sclerosis may, in part, be inherited (genetics contribute to the increased risk among family members). Siblings of an affected person have a 2% to 5% risk of developing MS.
Some scientists theorise that MS might stem from a combination of genetic factors and environmental triggers. It’s hypothesised that individuals may be born with a genetic predisposition, and upon exposure to specific environmental agents, an autoimmune response is triggered.
What are the types of Multiple Sclerosis?
Multiple Sclerosis (MS) is categorised into several types based on the patterns of disease progression and symptoms. The main types of multiple sclerosis include:
- Relapsing-Remitting Multiple Sclerosis (RRMS): Relapsing-remitting multiple sclerosis (RRMS) is the most common form of MS. It is distinguished by periodic relapses, causing temporary worsening of symptoms like fatigue, weakness, numbness, or coordination difficulties. After relapses, individuals have periods of partial or complete recovery, known as remissions, with no disease progression. Between relapses, individuals often experience improved symptoms and return to a baseline level of function.
- Primary Progressive Multiple Sclerosis (PPMS): It can encompass a range of neurological issues, such as mobility challenges, cognitive decline, and sensory impairments. The steady march of symptoms can be emotionally and physically demanding, requiring resilience and adaptability from those living with PPMS.
- Secondary Progressive Multiple Sclerosis (SPMS): Secondary progressive multiple sclerosis (SPMS) signifies a shift from the initial relapsing-remitting phase of MS. Following relapsing-remitting MS (RRMS), which involves distinct episodes of symptom exacerbation and recovery, individuals may transition to SPMS after a variable period. SPMS is marked by a more nuanced pattern of disease activity, with less frequent and severe relapses and minor, temporary remissions, distinguishing it from the distinct relapses and remissions seen in RRMS.
- Progressive-Relapsing Multiple Sclerosis (PRMS): PRMS is a relatively rare form of MS. It is indicated by a steadily worsening disease course from the onset, with occasional relapses and periods of partial remission. A steady accumulation of symptoms and disability marks this progressive decline. Unlike RRMS, the remissions in PRMS are usually incomplete, and disability accumulates over time. It’s important to note that while these types provide a general framework, the progression and symptoms of MS can vary widely between individuals. A healthcare professional specialising in neurology is best suited to diagnose and determine the specific type of MS based on an individual’s symptoms, medical history, and diagnostic tests.

Related reading: What Is Arthrogryposis?
Treatment for Multiple Sclerosis
Managing MS involves a comprehensive approach, with disease-modifying therapies (DMTs) crucial in altering the disease course by reducing relapse frequency and severity and slowing disability progression. DMTs are mainly used for “relapsing forms” like Relapsing-Remitting MS (RRMS). The absence of approved therapies for Primary Progressive MS (PPMS) without relapses emphasises the need for ongoing research. Scientists globally are actively exploring immunomodulatory agents, neuroprotective strategies, and remyelination therapies to provide effective treatments for progressive forms, addressing both symptoms and disease progression.
The prognosis for Multiple Sclerosis
The prognosis for multiple sclerosis typically involves a low risk of fatality, with a slight shortening of life expectancy. Concerns focus on quality of life and potential disability. After 15 years, fewer than 20% of individuals with MS are fully debilitated, while 20% may require mobility aids. Encouragingly, 60% remain ambulatory without assistance. Additionally, up to one-third experience minimal disability throughout life, highlighting the heterogeneous nature of MS. Advances in medical research offer hope for improved prognoses through better treatments and understanding of the disease’s mechanisms.
Mobility aids for people with Multiple Sclerosis
For individuals living with MS, approximately 30% may experience limitations in mobility that necessitate the use of a wheelchair, often opting for powerchairs to address challenges related to limited strength and fatigue.
Quantum Rehab powerchairs
Quantum Rehab, recognised as the global leader in individualised powerchair solutions, places a strong emphasis on developing mobility technologies specifically tailored to the unique needs of individuals with MS. Quantum powerchairs are designed to provide customisable solutions that enhance user comfort, repositioning, and overall independence. One key feature is the incorporation of power-adjustable seating, allowing users to modify their seating positions to find the most comfortable and functional arrangement. This adaptability is particularly valuable for individuals with MS, who may experience varying levels of fatigue and discomfort and changes in mobility over time.
Speciality drive controls are another crucial aspect of Quantum powerchairs. Recognising the diverse needs of individuals with MS, these powerchairs offer a range of control options. This includes advanced controls that enable users to operate the powerchair using a single finger or their head, catering to those with varying levels of motor function. Such innovative control mechanisms enhance accessibility and usability for individuals facing manual dexterity or muscle strength challenges.
The highly adaptable design of Quantum powerchairs is geared towards meeting the current and future needs of individuals with MS. This forward-thinking approach acknowledges the progressive nature of the disease and aims to provide a solution that can evolve alongside the user’s changing requirements. This adaptability ensures that the powerchair remains a relevant and effective mobility aid throughout the individual’s experience with MS.
Moreover, Quantum powerchairs incorporate the latest advanced technologies to further increase the independence of those living with MS. This may include features such as smart sensors, intelligent navigation systems, and connectivity options that enhance the overall user experience and contribute to more seamless integration of the powerchair into the user’s daily life.
iLevel seat elevation technology allows users to operate the powerchair seated or standing. Bluetooth is also integrated into Quantum’s Q-Logic 3 electronics, so those with multiple sclerosis can operate much of their environment with the powerchair drive control itself. Quantum powerchairs are designed to give those living with multiple sclerosis optimal medical comfort and maximum independence.
Related reading: 5 Tips for Selecting the Perfect Powerchair
Mobility and assistive technology needs
Depending on the progression and type of multiple sclerosis, mobility needs can include canes and crutches, leg braces, walkers, manual wheelchairs and scooters. Some people living with MS rely on a power mobility device to assist them with the performance of mobility-related activities of daily living (MRADLs). These individuals may be able to push a manual wheelchair for part of the day but, due to fatigue, also rely on a powered mobility product.
When someone with MS needs a power wheelchair, they are often recommended to choose a power base that can be easily adjusted to accommodate their evolving seating and electronics requirements. Starting with proportional control (joystick) is often advised initially, as it offers the most direct control for operating the power base. As MS progresses and the individual faces increased fatigue, muscle weakness, or other functionality challenges, specialised controls may become necessary to help them carry out everyday activities.
Optional LED fender lights on the Q6 Edge 3 help clients see and be seen. If the individual has decreased ability to shift weight independently or has developed altered sensation, the individual may require the benefits of a power positioning system. Options include tilt and recline systems, power seat elevation with iLevel and a power articulating foot platform.
Solution
When transitioning from a manual wheelchair to power mobility, choosing a power base that can accommodate full seating and positioning options and various drive controls is essential. The Q6 Edge 3 is compatible with a range of seating and positioning components, offering optional features like a 4.5 mph iLevel power-adjustable seat height and lifting clients to 12″ for enhanced independence and social interaction.
The Q6 Edge 3 Stretto is similarly versatile, boasting a wide selection of seating and positioning options and a strong reputation for quality and reliability. Both powerchairs can also be equipped with expandable electronics to adapt to changing needs.
Related reading: Choosing the Right Powerchair for You
Dubai Mobility is a guiding source of support and information for individuals confronting MS. It aligns with our vision to empower individuals throughout their journeys with multiple sclerosis. We are dedicated to offering personalised solutions that adapt to evolving needs and promote independence.
Contact Us
Enter Your Details: Provide your name, phone number and email.
Your Requirements: Let us know if you have any specific need or question
We’ll handle the rest: We’ll get back to you within 24 hours and provide the information you need.
World-class products – leading mobility brands











