What is Osteogenesis Imperfecta?
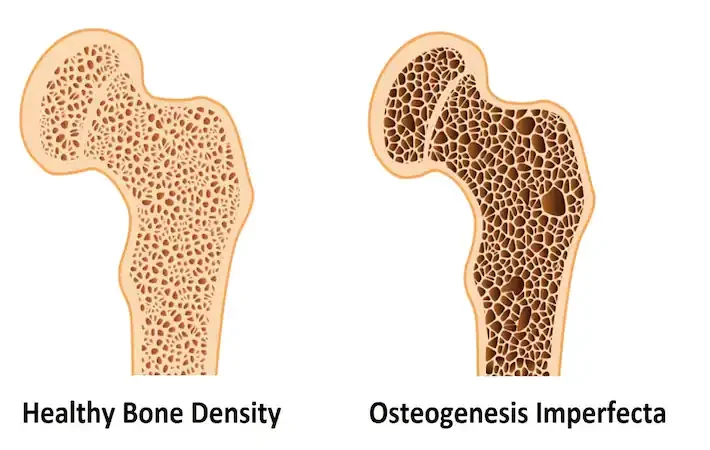
Osteogenesis Imperfecta (OI, or brittle bones disease) is a group of genetic disorders that mainly affect the bones. The term “Osteogenesis Imperfect” means imperfect bone formation. People with this condition have bones that break easily, often from mild trauma or without apparent cause. Multiple fractures are common and can occur even before birth in severe cases. Milder cases may involve only a few fractures over a person’s lifetime. Additional complications can involve hearing loss, heart failure, spine issues, and deformities. Osteogenesis imperfecta can sometimes be life-threatening if it occurs in babies either before or shortly after birth. Approximately one person in 20,000 will develop brittle bone disease. It occurs equally among males and females and ethnic groups.
What causes Osteogenesis Imperfecta?
Osteogenesis Imperfecta is caused by an abnormality in the gene that produces type 1 collagen, a protein used to create bone. The defective gene is usually. In some cases, however, a genetic mutation or change can cause it.

What are the symptoms of Osteogenesis Imperfecta?
Everyone with Osteogenesis Imperfecta has fragile bones. However, the severity of other symptoms varies, potentially including:
- Bone deformities
- Multiple broken bones
- Loose joints
- Weak teeth
- The blue sclera, or a bluish colour in the white of the eye
- Bowed legs and arms
- Kyphosis, or an abnormal outward curve of the upper spine
- Scoliosis, or an abnormal lateral curve of the spine
- Early hearing loss
- Respiratory problems
- Heart defects
Types of Osteogenesis Imperfecta
There are four primary types of Osteogenesis Imperfecta:
- Type 1 is the mildest and most common form. The body produces quality collagen, but not enough of it in this type. This results in mildly fragile bones. Children with Type 1 typically have bone fractures due to mild traumas. Such bone fractures are much less common in adults. The teeth may also be affected, resulting in dental cracks and cavities.
- Type 2 is the most severe form, and it can be life-threatening. In Type 2, the body either doesn’t produce enough collagen or produces collagen that’s poor quality. Type 2 can cause bone deformities. If born with Type 2, one may have a narrowed chest, broken or misshapen ribs, or underdeveloped lungs. Babies with Type 2 can die in the womb or shortly after birth.
- Type 3 is also a severe form. It causes bones to break easily. With Type 3, the child’s body produces enough collagen but its poor quality. The child’s bones can begin to break before birth. Bone deformities are common and may get worse as the child gets older.
- Type 4 is the most variable form because its symptoms range from mild to severe. As with Type 3, the body produces enough collagen, but the quality is poor. Children with Type 4 are typically born with bowed legs, although the bowing tends to lessen with age.
How is osteogenesis Imperfecta Diagnosed?
Osteogenesis Imperfecta is diagnosed by taking X-rays. X-rays allow doctors to see current and past broken bones. They also make it easier to view defects in the bones. Lab tests may be used to analyse the structure of a child’s collagen. In some cases, doctors may want to do a skin punch biopsy. The doctor will use a sharp, hollow tube to remove a small tissue sample during this biopsy. Genetic testing can be done to trace the source of any defective genes.
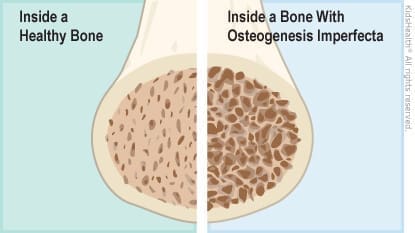
How is Osteogenesis Imperfecta treated?
There is no cure for Osteogenesis Imperfecta. However, treatment can relieve symptoms, prevent breakage of bones and maximize movement. Treatment may include:
- Splints and casts for broken bones
- Braces for weak legs, ankles, knees, and wrists
- Physical therapy to strengthen the body and improve movement
- Medicine to make the bones stronger
- Surgery to implant rods in the arms or legs
- Special dental work, such as crowns for brittle teeth
The prognosis for Osteogenesis Imperfecta
The long-term prognosis for those with Osteogenesis Imperfecta varies based on the type.
- Type 1 lives a typical lifespan, with few medical issues.
- Type 2 is often fatal before or shortly after birth.
- Type 3 can result in deformities, health issues, and a shorter lifespan.
- Type 4 may require such mobility aids as crutches, but lifespan is typical.
Most with Osteogenesis Imperfecta live socio-economic lives on par with the general population.
Mobility for those with Osteogenesis Imperfecta
For those with forms of Osteogenesis Imperfecta with mobility needs, a specialised power wheelchair, including smooth-riding suspension, is needed. Quantum Rehab, the global leader in individualised powerchairs, emphasises mobility technologies specific to the needs of those with Osteogenesis Imperfecta. Quantum powerchairs incorporate soft ride suspension to reduce pain from bumps and jarring; power-adjustable seating for user repositioning and comfort; specialty drive controls, including those requiring minimal hand strength; and a highly adaptable design to meet an individual’s current and future needs. Quantum powerchairs feature the latest advanced technologies to increase the independence of those living with Osteogenesis Imperfecta.
iLevel seat elevation technology allows users to operate the powerchair seated or standing. Bluetooth is also integrated into Quantum’s Q-Logic 3 electronics, so those with Osteogenesis Imperfecta can operate much of their environment with the power chair drive control. For those with Osteogenesis Imperfecta, Quantum powerchairs are designed to provide optimal medical comfort and maximum independence.
Solution
The Quantum Edge 3 with industry-first 4.5 mph at iLevel offers the most advanced powerchair experience. Q6 Powerchair series, which includes the Edge 3 and Q6 Edge 2 powerchairs, provide highly adjustable mid-wheel drive power bases. The Q6 Edge 2 all accept our optional iLevel technology, which offers up to 12 inches of lift at 4.5 mph. The 4Front is a quiet, more responsive front-wheel drive powerchair that features automotive-grade suspension with unprecedented comfort and rides quality.
Contact Us
Enter Your Details: Provide your name, phone number and email.
Your Requirements: Let us know if you have any specific need or question
We’ll handle the rest: We’ll get back to you within 24 hours and provide the information you need.
World-class products – leading mobility brands










